Smoking Impacts on Lung.
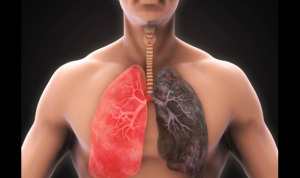
Smoking has significant and harmful effects on the respiratory system and the body as a whole. Here’s an overview of what happens to the lungs after smoking and the positive changes that occur when you quit:
Effects of Smoking on the Lungs:

Tar Buildup:
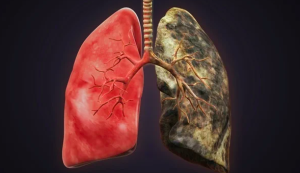
The term “tar” refers to the sticky, brown residue that is left behind in the lungs and airways when tobacco is smoked. This substance is a complex mixture of chemicals, including carcinogens (cancer-causing substances), and it is a major contributor to the negative effects of smoking on the lungs. Here’s how tar buildup affects the lungs:
Deposition in Airways:
When tobacco is burned, tar is released and inhaled into the lungs along with other smoke constituents. The tar contains numerous toxic substances, including polycyclic aromatic hydrocarbons (PAHs) and other chemicals.
Airway Obstruction:
Tar can accumulate on the walls of the bronchi and bronchioles, which are the large and small air passages in the lungs. Over time, this buildup can lead to the narrowing of the airways, making it more difficult for air to flow freely during breathing.
Reduced Lung Function:
The presence of tar in the lungs contributes to chronic inflammation and irritation. This can lead to conditions such as chronic bronchitis, where the airways are inflamed and produce excess mucus, further obstructing airflow. Reduced lung function is a hallmark of chronic obstructive pulmonary disease (COPD), which includes conditions like chronic bronchitis and emphysema.
Alveolar Damage:
Tar can also reach the alveoli, the tiny air sacs in the lungs where oxygen exchange takes place. The deposition of tar in the alveoli can cause damage and interfere with the exchange of oxygen and carbon dioxide.
Increased Risk of Respiratory Infections:
The presence of tar and other toxic substances in the lungs weakens the immune system’s defenses, making individuals more susceptible to respiratory infections like pneumonia and bronchitis.
Cancer Risk:
Many of the chemicals in tar are known carcinogens, and long-term exposure increases the risk of developing lung cancer. Tar contributes to the formation of cancerous cells in the lung tissue.
Environmental Advantages of Recycling Plastics.
Bronchoconstriction:
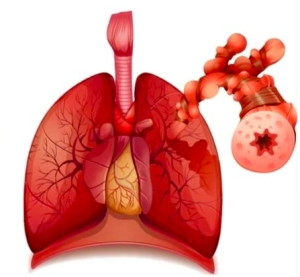
Bronchoconstriction refers to the narrowing of the air passages (bronchi and bronchioles) in the lungs. inhaling smoke has a direct impact on the respiratory system, leading to irritation and inflammation of the airways, which, in turn, can result in bronchoconstriction. Here’s how inhale smoke affects the lungs in terms of bronchoconstriction:
Irritation and Inflammation:
The chemicals present in cigarette smoke, including nicotine and various irritants, can irritate the lining of the airways. This irritation triggers an inflammatory response as the body attempts to defend itself against the perceived threat.
Smooth Muscle Constriction:
In response to the inflammation, the smooth muscle surrounding the airways may contract, leading to bronchoconstriction. This narrowing of the air passages makes it more difficult for air to flow in and out of the lungs, particularly during exhalation.
Increased Mucus Production:
Smoking also stimulates the production of excess mucus in the airways. The combination of bronchoconstriction and increased mucus can further obstruct the air passages, making breathing more challenging.
Chronic Bronchitis:
Long-term exposure to cigarette smoke can contribute to chronic bronchitis, a condition characterized by persistent inflammation of the bronchi and increased production of mucus. This chronic irritation and inflammation contribute to the narrowing of the airways.
Reduced Lung Function:
Bronchoconstriction, inflammation, and increased mucus production collectively lead to reduced lung function. This impairment in lung function is a key feature of chronic obstructive pulmonary disease (COPD), a progressive and debilitating respiratory condition associated with inhaling smoke.
Exacerbation of Asthma:
For individuals with asthma, inhaling smoke can exacerbate bronchoconstriction and worsen asthma symptoms. The combination of smoking and asthma can lead to more frequent and severe asthma attacks.
Increased Risk of Respiratory Infections:
The compromised airways are more susceptible to respiratory infections. Smoking weakens the immune system’s ability to defend against infections, leading to an increased risk of conditions such as pneumonia and bronchitis.
Reduced Ciliary Function:
Cilia are tiny hair-like structures found in the respiratory tract, including the bronchi and bronchioles, that play a crucial role in maintaining the health of the lungs. The coordinated movement of cilia helps to move mucus, along with trapped particles and microorganisms, out of the respiratory system. Smoking has detrimental effects on ciliary function, and here’s how:
Paralysis and Damage:
The chemicals in cigarette smoke can damage and paralyze the cilia. Over the long run, this harm impedes the cilia’s capacity to move in an organized way, diminishing their viability in cleaning bodily fluid and particles off of the aviation routes.
Increased Mucus Retention:
With reduced ciliary function, mucus produced in the airways is not efficiently cleared. This prompts an amassing of bodily fluid, which can add to aviation route hindrance and increase the gamble of respiratory diseases.
Risk of Chronic Bronchitis:
The impaired clearance of mucus due to reduced ciliary function contributes to the development of chronic bronchitis. Chronic bronchitis is characterized by persistent inflammation of the bronchi and increased mucus production.
Susceptibility to Infections:
Cilia assume a pivotal part in safeguarding against respiratory contaminations by assisting with eliminating microorganisms and trash. When ciliary function is compromised, the lungs become more susceptible to infections such as pneumonia and bronchitis.
COPD Progression:
Chronic obstructive pulmonary disease (COPD), a condition that includes chronic bronchitis and emphysema, is associated with long-term smoking. Reduced ciliary function contributes to the progression of COPD by allowing inflammation and mucus buildup to persist in the airways.
Slower Recovery from Respiratory Illnesses:
Smokers may experience a slower recovery from respiratory illnesses due to compromised ciliary function. The disabled capacity to clear bodily fluid can drag out side effects and increase the seriousness of respiratory diseases.
Inflammation and Infection:
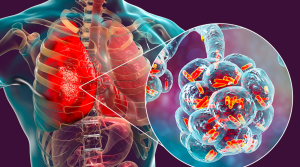
Smoking has significant and harmful effects on the lungs, particularly in terms of inflammation and increased susceptibility to respiratory infections. Here’s how inhaling smoke affects the lungs in terms of inflammation and infection:
Chronic Inflammation:
Smoking leads to chronic inflammation in the airways and lung tissue. The inhalation of toxic chemicals from cigarette smoke triggers an immune response, causing the release of inflammatory mediators. Prolonged inflammation contributes to tissue damage and structural changes in the lungs.
Airway Remodeling:
Chronic inflammation can lead to structural changes in the airways, a process known as airway remodeling. This remodeling may result in the thickening of airway walls, increased mucus production, and narrowing of the air passages. These changes contribute to airflow limitation and reduced lung function.
Reduced Immune Response:
Smoking weakens the immune system’s ability to respond effectively to infections. The function of immune cells in the lungs, such as macrophages and neutrophils, is compromised by exposure to cigarette smoke. This impaired immune response makes individuals more susceptible to respiratory infections.
Increased Risk of Respiratory Infections:
Smokers are at a higher risk of developing respiratory infections, including acute bronchitis, chronic bronchitis, and pneumonia. The combination of reduced ciliary function, impaired immune response, and chronic inflammation creates an environment conducive to bacterial and viral infections.
Exacerbation of Chronic Respiratory Conditions:
For individuals with pre-existing respiratory conditions such as asthma or chronic obstructive pulmonary disease (COPD), smoking can exacerbate inflammation and worsen symptoms. This can lead to more frequent and severe episodes of wheezing, coughing, and shortness of breath.
Impaired Wound Healing:
Smoking hinders the process of wound healing in the lungs. The chronic inflammatory state created by inhaling smoke can interfere with the repair of damaged lung tissue, making it more challenging for the respiratory system to recover from injuries.
Lung Cancer:
Long-term exposure to cigarette smoke is a major risk factor for lung cancer. The chronic inflammation caused by smoking contributes to the development of cancerous cells in the lung tissue.
Foods that support weight loss.
Emphysema:

Emphysema is a progressive and irreversible lung condition that is often associated with long-term smoking. It is a type of chronic obstructive pulmonary disease (COPD) characterized by damage to the air sacs (alveoli) in the lungs. Smoking is the primary cause of emphysema, and its effects on the lungs contribute to the development and progression of this condition. Here’s how inhaling smoke affects the lungs in the context of emphysema:
Alveolar Damage:
Smoking exposes the lungs to harmful chemicals, including irritants and toxins. Over time, chronic exposure to these substances damages the delicate walls of the alveoli, which are responsible for the exchange of oxygen and carbon dioxide in the lungs.
Loss of Elasticity:
The destruction of alveolar walls leads to the loss of elasticity in the lung tissue. Normally, the lungs expand and contract easily during breathing due to the elastic properties of the alveoli. In emphysema, this elasticity is compromised, making it difficult for the lungs to recoil and expel air effectively.
Air Trapping:
Emphysema results in the enlargement of air spaces within the lungs, primarily the alveoli. As a consequence, the air can become trapped in these enlarged spaces during exhalation. This leads to hyperinflation of the lungs and further impairs the ability to expel air, resulting in increased residual volume.
Difficulty Breathing:
The loss of lung elasticity and the destruction of alveoli make it progressively harder for individuals with emphysema to breathe. They may experience shortness of breath, especially during physical exertion, and over time, even simple activities like walking or climbing stairs can become challenging.
Chronic Cough:
Emphysema is often accompanied by chronic bronchitis, another form of COPD. Chronic bronchitis involves persistent inflammation and mucus production in the airways. The combination of emphysema and chronic bronchitis contributes to a chronic cough.
Reduced Exercise Tolerance:
As emphysema advances, individuals may experience a significant decline in exercise tolerance. This is due to impaired lung function, reduced oxygen exchange, and increased work of breathing.
Risk of Respiratory Infections:
Individuals with emphysema are at an increased risk of respiratory infections, such as pneumonia and bronchitis, due to compromised lung defenses and impaired clearance of mucus from the airways.
Positive Changes After Quitting Smoking:

Immediate Improvement:
Quitting smoking brings about immediate improvements to various aspects of health, even within a short period after cessation. Here are some positive changes that occur shortly after quitting smoking:
Improved Oxygen Levels:
Within hours of quitting, carbon monoxide levels in the blood begin to decrease. Carbon monoxide is a toxic gas present in cigarette smoke that competes with oxygen for binding to hemoglobin in red blood cells. As carbon monoxide levels drop, oxygen levels in the blood increase, leading to improved oxygen transport to vital organs and tissues.
Enhanced Lung Function:
The respiratory system starts to recover immediately after quitting. The bronchial tubes begin to relax, and lung function improves. This leads to increased airflow and ease of breathing.
Decreased Heart Rate and Blood Pressure:
Nicotine in cigarettes stimulates the release of adrenaline, which can elevate heart rate and blood pressure. Within the first day of quitting, the heart rate begins to decrease, and blood pressure starts to normalize.
Improved Circulation:
Smoking constricts blood vessels, leading to reduced blood flow. When inhaling smoke is stopped, blood vessels start to relax and widen, enhancing circulation throughout the body. This improved circulation benefits the heart, skin, and other organs.
Lowered Risk of Cardiovascular Events:
Quitting smoking immediately reduces the risk of cardiovascular events such as heart attacks and strokes. The positive changes in blood pressure, heart rate, and circulation contribute to a more heart-healthy state.
Enhanced Sense of Taste and Smell:
Smoking dulls the senses of taste and smell. Within days of quitting, these senses begin to sharpen, allowing individuals to enjoy food more and perceive scents more accurately.
Improved Respiratory Symptoms:
Smokers often experience respiratory symptoms such as coughing and shortness of breath. Within a few weeks of quitting, these symptoms tend to improve as the respiratory system starts to heal.
Reduction in Coughing and Wheezing:
The irritation caused by smoking can lead to chronic coughing and wheezing. After quitting, the airways begin to relax, and the frequency of coughing and wheezing typically decreases.
Better Skin Health:
Smoking accelerates skin aging and contributes to wrinkles. Stopping smoking elevates better bloodstream to the skin, decreasing the presence of kinks and advancing better coloring.
Cilia Functionality:
One of the positive changes that occur after quitting smoking is the improvement in cilia functionality. Cilia are little hair-like designs in the respiratory lot that assume a significant part in keeping up with lung wellbeing. The cilia’s fundamental capability is to move bodily fluid and cough particles out of the aviation routes, assisting with safeguarding the lungs from diseases and aggravations. Here’s how cilia functionality improves after quitting smoking:
A scientific way to reduce belly fat.
Recovery of Cilia:
Smoking damages and impairs the function of cilia in the airways. The chemicals in cigarette smoke interfere with the normal movement of cilia, reducing their effectiveness in clearing mucus and foreign particles. When a person quits inhaling smoke, the recovery process begins, and cilia gradually regain their ability to move.
Enhanced Mucus Clearance:
As cilia recover, the clearance of mucus from the respiratory tract becomes more efficient. This is important for maintaining a healthy airway environment by removing irritants, microbes, and debris. Improved mucus clearance contributes to a lower risk of respiratory infections.
Reduced Respiratory Irritation:
Cilia play a crucial role in preventing respiratory irritation by clearing away irritants that may otherwise lead to chronic inflammation. As cilia function improves, the risk of persistent irritation and inflammation in the airways decreases.
Lowered Risk of Respiratory Infections:
The recovery of cilia function enhances the lung’s defense mechanisms against infections. Productive bodily fluid leeway forestalls the development of irresistible specialists, decreasing the gamble of respiratory contaminations like bronchitis and pneumonia.
Improved Lung Health:
Restoring cilia functionality is a key aspect of overall lung health. Efficient cilia movement contributes to the maintenance of clear and healthy airways, supporting optimal respiratory function.
Reduced Inflammation:
Quitting smoking leads to various positive changes in the body, including a reduction in inflammation. Smoking is a significant reason for ongoing irritation, which is connected to various medical conditions. When a person quits smoking, the body undergoes a series of positive changes that contribute to a decrease in inflammation. Here’s how quitting inhaling smoke reduces inflammation:
Lowering Inflammatory Markers:
Smoking is related to expanded degrees of fiery markers in the blood, like C-receptive protein (CRP), and supportive of provocative cytokines. After quitting, these markers tend to decrease, indicating a reduction in systemic inflammation.
Improved Immune Response:
Smoking suppresses the immune system, making it less effective in responding to infections and injuries. When a person quits inhaling smoke, the immune system begins to recover, leading to a more balanced and robust response. This, thus, helps in diminishing constant aggravation.
Decreased Oxidative Stress:
Smoking generates oxidative stress in the body, causing an imbalance between antioxidants and reactive oxygen species. This oxidative pressure adds to aggravation and harm to tissues. Stopping smoking permits the body to reestablish this equilibrium, decreasing oxidative pressure and irritation.
Normalization of Blood Flow:
Smoking damages blood vessels and impairs blood flow, contributing to inflammation. When a person quits inhaling smoke, blood vessels start to recover, and blood flow improves. This restoration of normal vascular function helps in reducing inflammation throughout the body.
Less Tissue Damage:
Smoking is associated with damage to various tissues, including the lungs and cardiovascular system. As the body repairs itself after quitting, the extent of tissue damage decreases, leading to a reduction in inflammation.
Lower Risk of Chronic Diseases:
Ongoing provocative circumstances are risk factors for a few illnesses, including coronary illness, stroke, and certain tumors. By stopping smoking and diminishing aggravation, people bring down their gamble of fostering these serious ailments.
Improved Respiratory Health:
Smoking-induced inflammation in the respiratory system contributes to conditions such as chronic bronchitis and emphysema. Stopping inhaling smoke aides in lessening aviation route aggravation, prompting work on respiratory well-being.
Better Wound Healing:
Smoking delays wound healing by impairing the inflammatory response. After quitting, the body’s ability to mount an effective inflammatory response improves, facilitating better wound healing.
Improved Lung Function:

Quitting smoking leads to a range of positive changes in lung function, supporting the overall health of the respiratory system. Here are some of the improvements in lung function that occur after quitting inhaling smoke:
Increased Lung Capacity:
Smoking can cause damage to the lungs, leading to reduced lung capacity. After quitting, the lungs start to repair, and lung capacity may increase. This means that the lungs can hold more air, allowing for better oxygen exchange.
Improved Airflow:
Smoking can result in the narrowing of air passages due to inflammation and the buildup of mucus. Quitting inhaling smoke helps to reduce inflammation, allowing the airways to relax and open up. This improvement in airflow contributes to easier and more efficient breathing.
Enhanced Ciliary Function:
Cilia, the tiny hair-like structures in the airways, play a crucial role in clearing mucus and foreign particles. Smoking damages cilia, leading to impaired function. After quitting, ciliary function improves, facilitating the removal of mucus and reducing the risk of respiratory infections.
Reduced Respiratory Symptoms:
Smokers often experience respiratory symptoms such as coughing, wheezing, and shortness of breath. These symptoms tend to improve after quitting smoking as the respiratory system undergoes repair and inflammation decreases.
Decreased Risk of COPD:
Smoking is a major risk factor for chronic obstructive pulmonary disease (COPD), a progressive lung condition that includes chronic bronchitis and emphysema. Quitting inhaling smoke significantly lowers the risk of developing or worsening COPD.
Lowered Risk of Respiratory Infections:
Smoking weakens the immune system and damages the respiratory epithelium, making smokers more susceptible to respiratory infections. After quitting, the immune system becomes more robust, reducing the risk of infections such as bronchitis and pneumonia.
Enhanced Exercise Tolerance:
Quitting smoking can lead to improved cardiovascular fitness and endurance. As lung function improves, individuals often find that their ability to engage in physical activities increases, and exercise tolerance improves.
Reduction in Airway Hyperresponsiveness:
Smoking can increase airway hyperresponsiveness, making the airways more sensitive to irritants and causing symptoms such as coughing and wheezing. Quitting inhaling smoke helps in reducing airway hyperresponsiveness, leading to fewer respiratory symptoms.
Lowered Risk of Lung Cancer:
Quitting smoking is the most effective way to reduce the risk of lung cancer. The risk decreases over time after quitting, and the lungs have a better chance of recovering from the damage caused by smoking.
Decreased Risk of Cancer:

Quitting smoking is one of the most effective measures to reduce the risk of various types of cancer, particularly lung cancer. Here are the positive changes in cancer risk that occur after quitting smoking:
Decreased Risk of Lung Cancer:
Smoking is the primary cause of lung cancer, and quitting smoking significantly reduces the risk. The risk diminishes over time after quitting, even for individuals with a long history of inhaling smoke. After 10 years of cessation, the risk of lung cancer is approximately half that of a continuing smoker.
Lowered Risk of Other Cancers:
Smoking is associated with an increased risk of cancers in various organs, including the mouth, throat, esophagus, pancreas, bladder, cervix, and stomach. Quitting smoking reduces the risk of these cancers, and the risk continues to decrease with time after cessation.
Reduced Risk of Secondhand Smoke-Related Cancers:
Non-smokers exposed to secondhand smoke are at an increased risk of certain cancers. Quitting smoking not only benefits the individual smoker but also reduces the exposure of others to harmful substances in secondhand smoke, contributing to a decrease in their cancer risk.
Lowered Risk of Recurrence:
For individuals who have been diagnosed with and treated for cancer, quitting smoking is associated with a lower risk of cancer recurrence. Continued inhaling smoke after cancer treatment is linked to poorer outcomes and an increased risk of developing new cancers.
Improvement in Cellular Health:
Smoking damages DNA and promotes genetic mutations that can lead to the development of cancer. At the point when an individual stops smoking, the body’s cells start to fix and recuperate, lessening the gamble of additional DNA harm and changes related to disease.
How does sugar damage the brain?
Reversal of Premalignant Changes:
Smoking can cause precancerous changes in the cells lining the respiratory tract and other organs. Stopping smoking permits the body to invert a portion of these precancerous changes, decreasing the probability of disease improvement.
Beneficial Effects on Hormone-Related Cancers:
Smoking is associated with an increased risk of hormone-related cancers, such as breast and ovarian cancers in women. Stopping inhaling smoke can add to a decrease in this gamble.
Cardiovascular Benefits:

Quitting smoking brings about numerous cardiovascular benefits, leading to improvements in heart health and a reduction in the risk of cardiovascular diseases. Here are some positive changes that occur after quitting smoking in terms of cardiovascular health:
Improved Blood Circulation:
Smoking constricts blood vessels and reduces blood flow throughout the body. After quitting, blood vessels begin to relax and widen, leading to improved circulation. This conveys oxygen and supplements all the more productively to different organs and tissues.
Decreased Heart Rate:
Nicotine in cigarettes increases heart rate and blood pressure. After quitting, the heart rate gradually returns to a healthier and lower level, reducing the workload on the heart.
Lowered Blood Pressure:
Smoking raises blood pressure, contributing to the risk of heart disease and stroke. Halting smoking prompts a sluggish decrease in circulatory strain, progressing cardiovascular prosperity.
Normalization of Carbon Monoxide Levels:
Smoking introduces carbon monoxide into the bloodstream, which competes with oxygen for binding to hemoglobin. After quitting, carbon monoxide levels decline rapidly, allowing oxygen levels to normalize. This further develops the oxygen-conveying limit of the blood.
Reduced Risk of Blood Clots:
Smoking forms the bet of blood bunches, which can incite cardiovascular disappointments and strokes. Stopping smoking brings down the gamble of cluster development, decreasing the probability of cardiovascular occasions.
Improved Cholesterol Levels:
Smoking can negatively impact cholesterol levels, particularly by lowering high-density lipoprotein (HDL or “good” cholesterol). Quitting inhaling smoke contributes to a positive shift in cholesterol levels, with an increase in HDL cholesterol and a decrease in low-density lipoprotein (LDL or “bad” cholesterol).
Less Inflammation:
Smoking is associated with chronic inflammation, a factor contributing to atherosclerosis (hardening and narrowing of the arteries). After quitting, inflammation levels decrease, promoting healthier blood vessels.
Lowered Risk of Coronary Heart Disease:
Quitting smoking significantly reduces the risk of coronary heart disease, including conditions such as angina and heart attacks. The positive changes in circulatory strain, flow, and thickening gamble add to general cardiovascular well-being.
Enhanced Exercise Tolerance:
Quitting smoking improves cardiovascular fitness, leading to better exercise tolerance. Individuals often find it easier to engage in physical activities without experiencing shortness of breath and fatigue.
Reduced Risk of Peripheral Artery Disease (PAD):
Smoking is a major risk factor for PAD, a condition where blood flow to the extremities is restricted. Quitting inhaling smoke decreases the risk of PAD and improves blood flow to the legs and arms.
Enhanced Immune System:

Stopping smoking emphatically affects the resistant framework, improving the body’s capacity to guard against diseases and supporting in general well-being. Here are some of the positive changes that occur in the immune system after quitting smoking:
Improved Respiratory Immune Response:
Smoking compromises the immune defenses in the respiratory system, making individuals more susceptible to respiratory infections. After quitting, the immune system in the lungs becomes more effective at clearing pathogens, reducing the risk of conditions such as bronchitis and pneumonia.
Restoration of Immune Cell Function:
Smoking can impair the function of immune cells, including macrophages and neutrophils, which play crucial roles in recognizing and eliminating pathogens. Stopping inhaling smoke permits these invulnerable cells to recapture their typical capability, improving the body’s capacity to battle diseases.
Reduced Inflammation:
Chronic smoking induces systemic inflammation, which can contribute to various health problems. Stopping smoking prompts a decrease in irritation, permitting the resistant framework to work all the more productively and bringing down the gamble of fiery related illnesses.
Enhanced Antibody Production:
Smoking can affect the production of antibodies, and proteins that play a key role in recognizing and neutralizing pathogens. After quitting, the production of antibodies is restored, improving the body’s ability to mount an immune response against infections.
Lowered Risk of Infections:
Smoking debilitates the invulnerable framework, making people more helpless to diseases like colds, influenza, and respiratory contaminations. Stopping smoking diminishes the gamble of these diseases, and when they do happen, the insusceptible framework is better prepared to mount a powerful guard.
Improved Wound Healing:
Smoking can impair the process of wound healing by reducing blood flow and delaying the inflammatory response. Stopping smoking upgrades the resistant reaction associated with wound recuperating, prompting quicker and more successful recuperation from wounds or surgeries.
Reduced Autoimmune Risk:
Smoking is associated with an increased risk of autoimmune diseases, where the immune system mistakenly attacks the body’s tissues. Stopping smoking can assist with bringing down the gamble of creating immune system conditions.
Enhanced Vaccine Response:
Smoking can lessen the viability of immunizations by hindering the safe framework’s reaction. After stopping inhaling smoke, the safe framework turns out to be more responsive, working on the body’s capacity to create defensive antibodies in light of immunizations.
Decreased Risk of Chronic Diseases:
A strong immune system plays a vital role in preventing and controlling chronic diseases. Stopping smoking adds to in general safe framework well-being, diminishing the gamble of constant circumstances related to resistant brokenness.
Instagram Twitter Facebook LinkedIn Quora Google News
Our Other Engagements:





